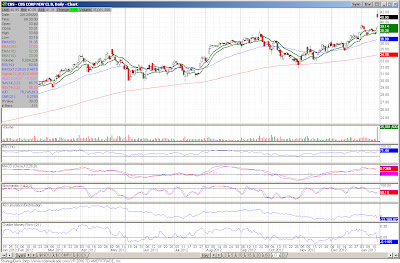
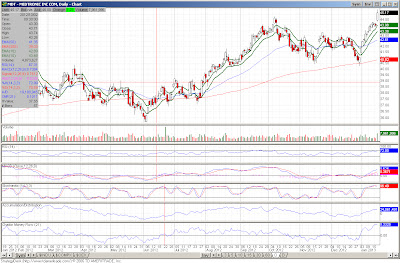
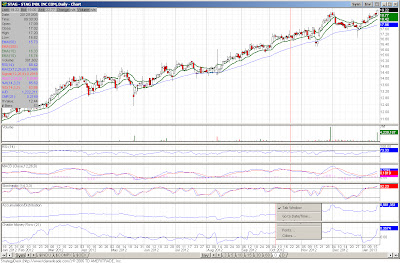
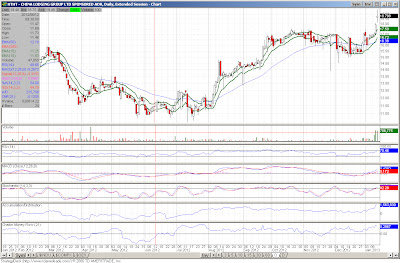
Quite a few names hitting the list today. One item of interest, seeing some strength in the broadcasting/advertising space with both CBS and LAMR making the list today. I also noticed at least one other name in the space making the screens despite it not making the visual criteria. Also seeing some strength in FITB, announcing better than expected earnings and the management stating the company had $1.5 billion in excess capital. Additionally, EBAY (which might as well be considered a bank with its Paypal unit) saw better earnings and the shareholders were rewarded. The small-cap stock FRGI was up nearly 7% on essentially no news. Ditto for HRB. This is while FUl reported better than expected earnings. Lastly, KSWS was sold to a Korean firm (so disregard the stock for any investment) and MDT's shares gained on an upgrade from the Street.
Health-insurance premiums have been rising—and
consumers will experience another series of price shocks later this year
when some see their premiums skyrocket thanks to the Affordable Care
Act, aka ObamaCare.
The reason: The congressional Democrats who crafted the legislation ignored virtually every actuarial principle governing rational insurance pricing. Premiums will soon reflect that disregard—indeed, premiums are already reflecting it.
Central to ObamaCare are requirements that health insurers (1) accept everyone who applies (guaranteed issue), (2) cannot charge more based on serious medical conditions (modified community rating), and (3) include numerous coverage mandates that force insurance to pay for many often uncovered medical conditions.
Guaranteed issue incentivizes people to forgo buying a policy until they get sick and need coverage (and then drop the policy after they get well). While ObamaCare imposes a financial penalty—or is it a tax?—to discourage people from gaming the system, it is too low to be a real disincentive. The result will be insurance pools that are smaller and sicker, and therefore more expensive.
How do we know these requirements will have such a negative impact on premiums? Eight states—New Jersey, New York, Maine, New Hampshire, Washington, Kentucky, Vermont and Massachusetts—enacted guaranteed issue and community rating in the mid-1990s and wrecked their individual (i.e., non-group) health-insurance markets. Premiums increased so much that Kentucky largely repealed its law in 2000 and some of the other states eventually modified their community-rating provisions.
States won't experience equal increases in their premiums under ObamaCare. Ironically, citizens in states that have acted responsibly over the years by adhering to standard actuarial principles and limiting the (often politically motivated) mandates will see the biggest increases, because their premiums have typically been the lowest.
Many actuaries, such as those in the international consulting firm Oliver Wyman, are now predicting an average increase of roughly 50% in premiums for some in the individual market for the same coverage. But that is an average. Large employer groups will be less affected, at least initially, because the law grandfathers in employers that self-insure. Small employers will likely see a significant increase, though not as large as the individual market, which will be the hardest hit.
We compared the average premiums in states that already have ObamaCare-like provisions in their laws and found that consumers in New Jersey, New York and Vermont already pay well over twice what citizens in many other states pay. Consumers in Maine and Massachusetts aren't far behind. Those states will likely see a small increase.
By contrast, Arizona, Arkansas, Georgia, Idaho, Iowa, Kentucky, Missouri, Ohio, Oklahoma, Tennessee, Utah, Wyoming and Virginia will likely see the largest increases—somewhere between 65% and 100%. Another 18 states, including Texas and Michigan, could see their rates rise between 35% and 65%.
While ObamaCare won't take full effect until 2014, health-insurance premiums in the individual market are already rising, and not just because of routine increases in medical costs. Insurers are adjusting premiums now in anticipation of the guaranteed-issue and community-rating mandates starting next year. There are newly imposed mandates, such as the coverage for children up to age 26, and what qualifies as coverage is much more comprehensive and expensive. Consolidation in the hospital system has been accelerated by ObamaCare and its push for Accountable Care Organizations. This means insurers must negotiate in a less competitive hospital market.
Although President Obama repeatedly claimed that health-insurance premiums for a family would be $2,500 lower by the end of his first term, they are actually about $3,000 higher—a spread of about $5,500 per family.
Health insurers have been understandably reluctant to discuss the coming price hikes that are driven by the Affordable Care Act. Mark Bertolini, CEO of Aetna, the country's third-largest health insurer, broke the silence on Dec. 12. "We're going to see some markets go up by as much as 100%," he told the company's annual investor conference in New York City.
Insurers know that the Obama administration will denounce the premium increases as the result of greedy health insurers, greedy doctors, greedy somebody. The Department of Health and Human Services will likely begin to threaten, arm-twist or investigate health insurers in an effort to force them into keeping their premiums more in line with Democratic promises—just as HHS bureaucrats have already started doing when insurers want premium increases larger than 10%.
And that may work for a while. It certainly has in Massachusetts, where politicians, including then-Gov. Mitt Romney, made all the same cost-lowering promises about the state's 2006 prequel to ObamaCare that have yet to come true.
But unlike the federal government, health insurers can't run perpetual deficits. Something will have to give, which will likely open the door to making health insurance a public utility completely regulated by the government, or the left's real goal: a single-payer system.
Mr. Matthews is a resident scholar with the Institute for Policy Innovation in Dallas, Texas. Mr. Litow is a retired actuary and past chairman of the Social Insurance Public Finance Section of the Society of Actuaries.
The reason: The congressional Democrats who crafted the legislation ignored virtually every actuarial principle governing rational insurance pricing. Premiums will soon reflect that disregard—indeed, premiums are already reflecting it.
Central to ObamaCare are requirements that health insurers (1) accept everyone who applies (guaranteed issue), (2) cannot charge more based on serious medical conditions (modified community rating), and (3) include numerous coverage mandates that force insurance to pay for many often uncovered medical conditions.
Guaranteed issue incentivizes people to forgo buying a policy until they get sick and need coverage (and then drop the policy after they get well). While ObamaCare imposes a financial penalty—or is it a tax?—to discourage people from gaming the system, it is too low to be a real disincentive. The result will be insurance pools that are smaller and sicker, and therefore more expensive.
How do we know these requirements will have such a negative impact on premiums? Eight states—New Jersey, New York, Maine, New Hampshire, Washington, Kentucky, Vermont and Massachusetts—enacted guaranteed issue and community rating in the mid-1990s and wrecked their individual (i.e., non-group) health-insurance markets. Premiums increased so much that Kentucky largely repealed its law in 2000 and some of the other states eventually modified their community-rating provisions.
States won't experience equal increases in their premiums under ObamaCare. Ironically, citizens in states that have acted responsibly over the years by adhering to standard actuarial principles and limiting the (often politically motivated) mandates will see the biggest increases, because their premiums have typically been the lowest.
Many actuaries, such as those in the international consulting firm Oliver Wyman, are now predicting an average increase of roughly 50% in premiums for some in the individual market for the same coverage. But that is an average. Large employer groups will be less affected, at least initially, because the law grandfathers in employers that self-insure. Small employers will likely see a significant increase, though not as large as the individual market, which will be the hardest hit.
We compared the average premiums in states that already have ObamaCare-like provisions in their laws and found that consumers in New Jersey, New York and Vermont already pay well over twice what citizens in many other states pay. Consumers in Maine and Massachusetts aren't far behind. Those states will likely see a small increase.
By contrast, Arizona, Arkansas, Georgia, Idaho, Iowa, Kentucky, Missouri, Ohio, Oklahoma, Tennessee, Utah, Wyoming and Virginia will likely see the largest increases—somewhere between 65% and 100%. Another 18 states, including Texas and Michigan, could see their rates rise between 35% and 65%.
While ObamaCare won't take full effect until 2014, health-insurance premiums in the individual market are already rising, and not just because of routine increases in medical costs. Insurers are adjusting premiums now in anticipation of the guaranteed-issue and community-rating mandates starting next year. There are newly imposed mandates, such as the coverage for children up to age 26, and what qualifies as coverage is much more comprehensive and expensive. Consolidation in the hospital system has been accelerated by ObamaCare and its push for Accountable Care Organizations. This means insurers must negotiate in a less competitive hospital market.
Although President Obama repeatedly claimed that health-insurance premiums for a family would be $2,500 lower by the end of his first term, they are actually about $3,000 higher—a spread of about $5,500 per family.
Health insurers have been understandably reluctant to discuss the coming price hikes that are driven by the Affordable Care Act. Mark Bertolini, CEO of Aetna, the country's third-largest health insurer, broke the silence on Dec. 12. "We're going to see some markets go up by as much as 100%," he told the company's annual investor conference in New York City.
Insurers know that the Obama administration will denounce the premium increases as the result of greedy health insurers, greedy doctors, greedy somebody. The Department of Health and Human Services will likely begin to threaten, arm-twist or investigate health insurers in an effort to force them into keeping their premiums more in line with Democratic promises—just as HHS bureaucrats have already started doing when insurers want premium increases larger than 10%.
And that may work for a while. It certainly has in Massachusetts, where politicians, including then-Gov. Mitt Romney, made all the same cost-lowering promises about the state's 2006 prequel to ObamaCare that have yet to come true.
But unlike the federal government, health insurers can't run perpetual deficits. Something will have to give, which will likely open the door to making health insurance a public utility completely regulated by the government, or the left's real goal: a single-payer system.
Mr. Matthews is a resident scholar with the Institute for Policy Innovation in Dallas, Texas. Mr. Litow is a retired actuary and past chairman of the Social Insurance Public Finance Section of the Society of Actuaries.